April 10, 2026
Foot Pain Warning Signs: What Your Feet May Be Trying to Tell You
Key Takeaways
-
Listen to your feet. Symptoms like persistent pain, numbness, burning, swelling, or skin and nail changes can be signs of developing foot conditions, not just typical daily aches. Keep a basic checklist to record the location of the pain, its duration, and the sensation.
-
Tell normal post-activity aches apart from something more serious by paying attention to duration, severity, and effect on daily activities. Pain that is sharp, frequent, or interrupts walking, balance, or sleep are warning signs not to be brushed off.
-
Be alert to structural shifts in your feet such as flattening or very high arches, new lumps or bumps, or shifting toe positions. These changes can impact your gait and result in long-term instability or deformity. Take note of when these changes started and any recent trauma or new shoes that may be associated.
-
Remember that foot pain, swelling, or wounds that won’t heal can occasionally indicate broader health concerns like diabetes, arthritis, or circulation. If you observe accompanying symptoms such as fatigue, fever, or leg pain, your feet might be warning you about a systemic issue.
-
Safeguard your foot health with proactive habits such as supportive, well-fitted shoes, consistent stretching and strengthening, and weekly inspections of skin, nails, and foot shape. These easy steps will prevent injuries, catch problems early, and support long-term mobility.
-
Look for a podiatrist or foot specialist evaluation if symptoms are persistent, worsening, or getting in the way of standing, walking, or exercising. Early diagnosis and a tailored treatment plan, which may involve orthotics, physical therapy, or other interventions, can minimize complications and aid recovery.
Foot pain warning signs are your first hints that something in your feet, ankles, or lower legs require attention and more diligent care. They typically manifest as piercing or aching pain, swelling, redness, warmth, dead spots or rigid joints that feel exacerbated by periods of standing or walking. Others foreshadow stress fractures, tendon strain, nerve issues or joint damage that can alter your gait. Other indicators, such as slow-healing sores or skin discoloration, can be associated with diabetes or blood flow concerns. To help distinguish between which signs are mild and which require quick attention, the following sections separate common patterns, causes, and when to seek medical attention.
Decoding Your Foot Pain Warning Signs
Foot pain creeps in and its early symptoms can be subtle and easy to overlook. Reading these signals in time saves you from long-term issues, loss of mobility, and more invasive treatment down the road.
1. Persistent Pain
Constant aching in the heel, arch, or toes is among the sharpest early warnings. We frequently attribute heel pain to plantar fasciitis, Achilles tendonitis, or heel spurs if it’s worse with the first steps in the morning or after prolonged standing. Arch pain can be caused by flat feet, high arches, or shoes that are worn out and no longer conform to your foot shape. Pain in the ball of the foot may indicate Morton’s neuroma, a benign nerve growth located between the third and fourth toes that can feel as if you are standing on a pebble.
It helps to document what alleviates or exacerbates the pain. If it spikes when you walk or run, then lingers even when you rest, it could be a stress fracture or tendonitis, not just the aches of the long day. Light, brief soreness after abnormal activity is normal, but don’t dismiss sharp, stabbing, or throbbing pain that alters your gait, causes limping, or wakes you up at night.
It’s helpful to chart trends. Record where it hurts (heel, arch, toes, ball of foot), duration, and intensity on a basic 0 to 10 scale. If you stand all day for work or train regularly, mark shifts or workouts alongside your pain level to determine if overuse is the primary culprit.
2. Sensory Changes
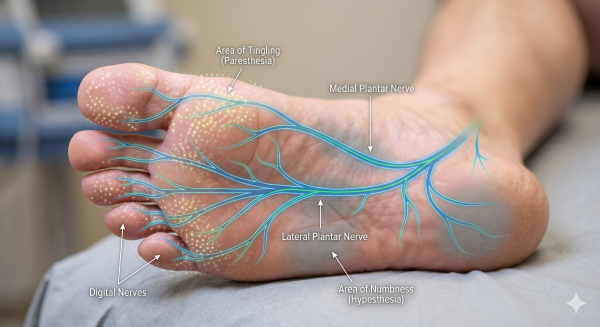
Sensation changes tend to indicate nerve or circulation issues, as opposed to mere strain. Numbness, tingling, or burning in the toes or sole may be associated with nerve damage, peripheral neuropathy, or a trapped nerve like Morton’s neuroma. A burning or electric shock sensation, particularly in the ball of the foot, warrants close attention.
Numbness, or the reverse — hypersensitivity to slight pressure — can appear in people with diabetes or circulatory issues. Perhaps you experience numbness, can’t sense small injuries, or feel an unusual pain when bed sheets brush the skin. If these changes are accompanied by weakness, foot drop, or frequent tripping, it can indicate more advanced nerve problems.
A simple way to keep track is to log what you feel and where:
|
Area affected |
Type of change |
Duration / pattern |
|---|---|---|
|
Toes |
Numb, tingling |
Off and on during the day |
|
Ball of foot |
Burning, sharp pain |
While walking or running |
|
Whole foot |
Reduced sensation |
Constant, worse at night |
Bring notes like these to a doctor or podiatrist so they can correlate your story with exam findings and tests.
3. Visual Alterations
Your feet display trouble on the skin before you experience major pain. Swelling around the ankle or top of the foot, redness over a joint, or dark patches on the toes can indicate inflammation, infection, a sprain, or sometimes a blood clot. One foot appearing much larger or warmer than the other is a red flag and should be examined immediately.
Skin changes count. Thick calluses that accumulate in one area, cracks that won’t heal, or open sores and ulcers – particularly in individuals with diabetes or compromised circulation – can evolve into threatening infections. Light or dark color changes, shiny skin, or hair loss on the toes occasionally tie to circulation problems.
Toenails speak their own language as well. Ingrown nails cause swelling and sharp edge pain. Yellow, crumbly nails lead to fungal infection and black or blue nails can be the result of trauma, like tight shoes or heavy impact. Bony bumps at the base of the big toe, known as bunions, or bent, claw-like toes, known as hammertoes, are warning signs that the architecture of your foot is changing and may begin to impact your stride.
Taking photos over weeks can help you notice slow changes in color, swelling, or shape that are hard to catch from day to day.
4. Structural Shifts
Alterations in your foot’s construction typically manifest prior to excruciating pain. New lumps on the top of the foot, a bump at the back of the heel, or toes that start to cross or curl under can each indicate bone spurs, tendon problems or early deformities. Sometimes these shifts relate to old injuries, and sometimes they arise from years of tight or narrow shoes that squish the toes.
Just listen to your arch line when you stand. Arches that flatten can cause flat feet, and very high arches push more weight onto the heel and ball of the foot. Either pattern can alter your stride and overload specific joints, leading to persistent wear. If your feet are stiff in the morning, or your toes don’t bend or straighten as much as they used to, arthritis or tendon issues may play a role in the picture.
It’s useful to note when you first observed a shift and what else changed around that time, such as new shoes, a training volume spike, weight gain, or a recent fall. This allows a clinician to better connect your symptoms to probable causes and select the appropriate combination of rest, support, or additional testing.
5. Functional Decline

Warning signs aren’t just visual or physical. They reveal themselves in the things you can no longer do effortlessly. If walking a few hundred meters, climbing stairs, or standing in line begins to cause foot pain, achiness, or burning that was not there before, it could be more than just tiredness. Those who stand all day or lead very active lifestyles tend to shrug this off as par for the course. A gradual decrease in what your feet can handle is critical information.
Losing your balance or tripping often can indicate weakness in the small muscles of the foot or ankle, nerve issues, or immobile joints. Perhaps you observe you shy away from uneven terrain or constantly favor one side. If you can’t bear weight on one foot, push off the ground, or develop a very evident limp that persists beyond a few days, that can indicate stress fractures, severe tendonitis, or joint damage.
Gait changes are important even if pain is minimal. A tiny limp, toeing one foot out or taking shorter steps on one side redirects stress to your knees, hips and back, which can escalate the issue upward. Jotting down when in the day your function dips, what shoes you wear, and what activities are most challenging provides a useful checklist you can consult independently and then share with a specialist.
Foot pain from overuse or mild strain frequently settles down with rest, ice, compression and elevation, light stretching and OTC pain medications. If pain, numbness, swelling, or function continue worsening over days or weeks despite these steps, or if you suspect a blood clot or serious injury, prompt medical care is necessary to rule out underlying issues such as fractures, severe arthritis, or peripheral neuropathy and safeguard long-term mobility.
When Pain Signals Systemic Issues
Foot pain isn’t always just an overuse issue. More often, it indicates problems with the nerves, circulation, joints, or immune system. By observing patterns, onset speed, and other body symptoms, you can distinguish between a local strain and a systemic disease requiring immediate attention.
When foot pain or swelling is caused by one of these issues, it’s usually a sign of something more systemic. Persistent, aching foot pain with morning stiffness, swollen joints and heat could indicate inflammatory arthritis like rheumatoid arthritis or gout. Toe, foot, or ankle pain with warmth and distinct redness can indicate cellulitis, crystal-induced arthritis, or infectious arthritis, particularly if accompanied by fever or malaise. Painful feet with tingling or “pins and needles” often indicate peripheral neuropathy. It can be local, but is common in diabetic neuropathy, where elevated blood sugar levels damage nerves and small blood vessels over time.
Unexplained patterns provide hints about nerve or spine issues. Pain or paresthesias in the leg and foot, particularly foot and low back pain elicited on straight leg raising and relieved on knee flexion, may be indicative of sciatica or lumbosacral radiculopathy. Numbness and pain around the ankle and heel, or tarsal tunnel syndrome, are more common in individuals with chronic swelling and can be associated with hypothyroidism. These symptoms indicate trouble somewhere other than the foot — in the spine, nerve tunnels, or hormone balance.
Changes in blood flow are another important warning sign. Ischemia, or poor blood supply, can manifest as cramping, aching, or cold pain in the foot and can be a reflection of peripheral artery disease or other heart and vessel disorders. Pain at rest, worse on elevation of the feet and relieved by letting them dangle, can suggest end-stage peripheral artery disease. Acute, severe foot pain that achieves maximal intensity within seconds or minutes, particularly in an AFib patient, can signify embolic arterial occlusion, which is an emergency. Episodic, very red, hot, burning feet can point to erythromelalgia, which is sometimes associated with blood or autoimmune disorders.
Differentiating Everyday Aches
Foot pain is prevalent. Not all pains signal big trouble. The trick is to distinguish short-term, activity-related soreness from pain that recurs, worsens, or begins to alter your lifestyle.
It’s your garden variety ache, which tends to manifest in the aftermath of a long walk, a run, or a day spent standing. Muscles ache, the feet might throb a little at night, and it all goes away with rest, elevating the feet, some light stretching, or a warm bath. This pain tends to dissipate within less than 24 to 48 hours and doesn’t trap you in a stiff or weird gait. It is often linked to clear triggers: new shoes that are too tight, thin soles with little cushion, a sudden jump in training distance, or minor bumps and twists that settle on their own.
Persistent or sharp pain is more of a red flag. If the pain persists for more than a few days, occurs most days of the week, or you wake at night because of it, the cause may lie in the joints, tendons, nerves, or bones. For instance, heel and arch pain that is worse with the first steps in the morning can indicate plantar fasciitis. Pain at the back of the heel that flares with running or stair climbing can indicate Achilles tendonitis from repetitive use of the tendon and calf muscles. If you are experiencing burning pain in the ball of your foot that may shoot into your toes, it can be Morton neuroma, a nerve problem that tighter shoes or high heels can exacerbate.
Location counts. Pain under the big toe joint can be from sesamoiditis, where the small sesamoid bones underneath that joint become irritated, frequently in runners, dancers, and those who do a lot on the balls of their feet. Pain in the ball of your foot could be Morton neuroma, a stress fracture, or joint strain. Numbness, tingling, or shooting pain down the inside of your ankle and into your sole can indicate tarsal tunnel syndrome, in which a nerve in your ankle is being compressed. Bent toes that rub in shoes can be hammertoes, loose, flexible ones in the beginning, but hard, fixed, and very painful over time.
A simple way to sort out normal aches from warning signs is to look at duration, severity, and impact on daily life:
|
Feature |
More Likely Normal Ache |
Possible Warning Sign |
|---|---|---|
|
Duration |
Eases within 1–2 days |
Lasts more than a week or keeps coming back |
|
Severity |
Mild, dull, settles with rest |
Sharp, burning, or severe, may wake you at night |
|
Impact on daily life |
You can walk and work with minor discomfort |
You limp, avoid weight bearing, or stop usual activities |
|
Trigger |
Clear cause (new workout, long day on feet) |
No clear cause, or pain grows even after cutting back activity |
|
Response to simple care |
Better with rest, ice, or shoe change in 24–48 hours |
Little or no change with basic home care |
The Risk of Ignoring Symptoms
To ignore persistent foot pain or changes in appearance or mobility is very likely to turn an acute problem into a chronic one. Foot pain is common, particularly after the age of 50, but ‘common’ doesn’t mean ‘harmless.’ Around 20% of seniors experience chronic foot pain, and a lot of it is connected to wear and tear that was never caught early. When it’s shunted aside, people begin to adjust their gait to compensate, which can strain knees, hips, and back and gradually erode everyday mobility.
Ignoring foot ailments increases the likelihood that pain will become a chronic issue. That could show up as morning stiffness, pain after a brief walk, or swelling that doesn’t fully subside. Eventually, something that began small like bunions, hammertoes, or plantar fasciitis can change the shape of the foot. This can result in deformity, which requires special shoe orthotics, braces, or surgery to fix. When patients wait too long for a provider to see them, recovery can extend six to eight weeks or longer, often with severe rest that interrupts work, exercise, and family life.
Early warning signs matter because they can mask something more serious. Your chronic foot pain could signal arthritis, nerve issues, insufficient blood circulation, or diabetes. Sometimes, calluses crack or little cuts that don’t heal can become ulcers or infections. Reduced sensation in the feet means that minor cuts and injuries can easily go unnoticed, putting diabetic people at risk of nerve damage or deep tissue complications. Some don’t even know they have a foot condition, which is why regular checks and taking new symptoms seriously are helpful.
Possible consequences of delayed treatment include:
-
Longer, more painful recovery
-
Higher risk of infections or ulcers
-
Stress fractures that need MRI and rest to heal
-
Lasting deformity and need for surgery
-
Reduced mobility and lower quality of life
Proactive Foot Health Strategies
Proactive care reduces the likelihood that minor warning signs become chronic foot issues. Simple daily habits, smart shoe choices, and regular self-checks often make the biggest difference.
-
Wash and dry your feet daily, including between the toes, to minimize moisture and reduce infection risk.
-
Hydrate dry skin, but never apply cream between your toes, where additional moisture can result in fungal problems.
-
Cut your toenails straight across and not too short. This can prevent ingrown toenails and painful nail edges.
-
Sit and stand in alternating intervals throughout the day to distribute load on the feet rather than to maintain pressure in one location.
-
Give your feet a break and when you can, elevate them above hip level to reduce swelling after long days.
-
Keep your weight in check because every additional kilo delivers consistent stress on joints, arches and the forefoot.
-
Once or twice a week, soak your feet in warm water with Epsom salt for 20 minutes to alleviate mild soreness and tightness.
Footwear
Shoe selection establishes the daily stress baseline for feet. Shoes with appropriate arch support and heel counters, as well as padding suitable for your activity level and weight, are important. A wide toe box provides room for toes to spread, which reduces pressure on nails, joints, and nerves.
As for length, shoot for at least 1.25 cm of space between your longest toe and the front of the shoe. This additional room reduces the risk of bruised nails, blisters, and forefoot pain when you walk or run. Don’t wear shoes that pinch, rub, or cram your foot into a tight shape.
Cut down on the time in high heels, pointed dress shoes, or compression-camping athletic shoes, as they can accelerate bunions, hammertoes, and nerve irritation. Alternate between pairs so the same crushing pattern doesn’t pummel your feet daily, and retire shoes once soles flatten or lean to one side.
A simple checklist helps: check toe room, arch support, heel grip, insole cushioning, outsole wear, and shoe weight. If one of them feels ‘off’, that pair might not be a great daily option.
Movement
Even simple, regular movement promotes circulation and strengthens foot tissues. Low-impact exercises like brisk walking, swimming, or cycling tend to work well for most people and they’re easier on joints than running or jumping sports. In my experience, brief daily walks sprinkled through the day usually treat the feet better than one hard go.
Targeted work provides an additional buffer. Easy exercises such as picking up a towel with your toes, rolling a ball beneath your arch, or slow calf raises strengthen the minor muscles that support the arch and assist in managing each step. Stretching matters: stand at arm’s length from a wall with hands on it and both feet on the floor, then lean forward to stretch the calves and the bottom of the feet.
Balance and flexibility exercises decrease your fall risk and improve your ability to adapt to uneven terrain. One simple example is to stand on one foot for 10 to 20 seconds while brushing your teeth or cooking. Then switch sides and repeat a few times. This silent drill supports ankle stability and joint proprioception without any overhead gear.
High-impact activity still serves a purpose, but pounding out long runs on unforgiving surfaces or endlessly hopping in place can aggravate preexisting pain or lead to overuse strains. When warning signs start, trim impact, introduce more rest days, and emphasize low-impact cross-training until symptoms subside.
Inspection
Routine screenings catch issues before they impact your stride. Check for blisters, calluses, cuts, cracked heels, skin discoloration, and any change in nail shape or thickness. Even tiny hot spots can be an indicator of rubbing, infection, or pressure from your gait.
Use a hand mirror for the soles and between toes, or have a partner or family member assist you if you have difficulty bending, poor vision, or decreased sensation in your feet. This holds true particularly for individuals with diabetes or neuropathy, conditions in which minor injuries might not cause pain but remain significant.
Record any new swelling, redness, warmth, or changes in toe position in a notebook or phone app. Noting patterns across weeks helps you identify what correlates to marathon work days, new footwear, or increased activity.
Schedule a weekly reminder, maybe alongside nail trimming or a scheduled foot soak, so that inspections become a regular part of your care routine instead of something you only do when the ache is already intense.
Seeking Professional Diagnosis
Foot pain that lingers is not “normal,” even if it feels slight. When it persists for weeks or begins to affect your posture or basic movements, it’s a cue for a professional diagnosis, not guesswork around the house.
Booking an appointment with a skilled podiatrist or foot doctor gives you a full clinical exam instead of guess-based self-care. A podiatrist will look at how you stand and walk, test your range of motion, press on key spots in the foot and ankle, and check your skin and toenails. This matters because problems in toenails, like thickening, color change, or recurring ingrown edges, can point to fungal infections, circulation issues, or pressure problems in your shoes. People who find it hard to stand for long, walk more than a few hundred meters, or climb stairs because of foot pain should treat that as a clear sign to see a podiatrist and not push through the pain.
When symptoms keep returning, get worse, or persist for weeks or months, it’s reasonable to inquire about diagnostic tests. X-rays can reveal stress fractures, bone spurs, or joint damage. Gait analysis can detect bad foot alignment or uneven weight load that could be causing heel pain or knee strain. Nerve studies assist when there is burning, tingling, or numb spots that can indicate nerve entrapment or diabetic nerve problems. These tests provide a more accurate diagnosis so treatment is rooted in actual evidence, not guesswork.
Once your podiatrist has a clear diagnosis, they can talk you through a plan that fits your life and health. This might begin with rest, ice, shoe changes, and anti-inflammatory medicine. Several see advantages from personalized orthotic inserts that support level feet, high arches, or agonizing heels. Others may require physical therapy to strengthen, balance, and safeguard weak joints. If you live with diabetes or have chronic foot problems, annual visits to the podiatrist catch subtle changes early, before they escalate into ulcers, ankle sprains, or persistent pain that inhibits your activities. A proper diagnosis and early treatment can stave off permanent injury and keep you moving.
Conclusion
Foot pain spells it out. Sharp heel jabs, deep arch burn, numb toes, night pain, or pain that radiates — they all tell a tale. Brief sore feet from a long walk feel normal. Pain that lingers, intensifies, or alters your stance or gait requires real attention.
Early checks save you time, stress, and money. Most foot problems remain mild with rest, ice, improved footwear, and basic stretches. Others are connected to bigger health problems, such as diabetes or arthritis, and require immediate evaluation.
As for next steps, maintain a quick pain log, record triggers, and schedule an appointment with a foot specialist if symptoms align with the red flags you encountered here. Your feet support you every day. Treat them as if they matter.
Frequently Asked Questions
What are the most common warning signs that foot pain is serious?
Look out for pain that is sharp, new, or worsening. Other red flags include swelling, redness, warmth, numbness, or changes in skin color or shape. If pain makes walking difficult or awakens you at night, see a podiatrist.
How can I tell normal foot aches from a medical problem?
Normal aches get better with rest, gentle stretching, and comfortable shoes. Concerning foot pain goes beyond everyday aches if it persists for more than a few days, recurs frequently, or is accompanied by swelling, stiffness, or numbness. If foot pain restricts your daily activity or exercise, have it checked.
Can foot pain be a sign of a health condition in the whole body?
Foot pain warning signs can indicate diabetes, arthritis, nerve issues, circulation problems, or an autoimmune disease. Tingling, burning, or slow-healing sores are all red flags. If you’re experiencing these symptoms, particularly in conjunction with pre-existing medical conditions, see a physician without delay.
What happens if I ignore ongoing foot pain?
If you ignore foot pain, it can result in chronic pain, joint damage, deformity, and mobility restrictions. You might alter your walk to circumvent pain, which can then damage your knees, hips, or back. Earlier diagnosis generally translates to easier, more effective treatment.
When should I see a doctor or podiatrist for foot pain?
Visit a specialist if pain persists beyond 5 to 7 days, is intense, occurs post-trauma, or is associated with swelling, fever, wounds, or discoloration. Get help if you have diabetes, poor circulation, or nerve disease and develop any new foot symptoms.
What proactive steps can I take to protect my foot health?
Wear well fitting, supportive footwear. Stay in shape. Stretch feet and calves. Don’t do too much too soon. Inspect your feet every day for signs of redness, blisters, or callouses, particularly if you are diabetic. Consult early if it feels weird.
Can I treat foot pain at home, and when is that not safe?
Mild overuse pain usually gets better with rest, ice, elevation, and good supportive shoes. Don’t depend on home care if the pain is severe or abrupt, or associated with a fall, if you can’t bear weight, or if you notice infection symptoms. In those instances, seek treatment.
Still searching for the right foot care solution? Explore Edmonton Foot Clinic’s most requested treatments for expert diagnosis, personalized prevention plans, and advanced podiatric care in Edmonton.
For additional trusted information on foot health and lower limb care, browse these external resources:

