January 23, 2026
Key Takeaways
-
Ingrown toenails can be caused by bad habits like poor trimming, tight shoes, repeated toe injury, and genetics. They can be exacerbated by health conditions that slow healing. Know the warning signs: redness, swelling, drainage, or severe pain, and get care early.
-
Wear footwear with plenty of room in the toe box and good support to relieve pressure on nail edges. Rotate your shoes, don’t wear tight socks all day long, and don’t wear high heels or pointy shoes all the time.
-
So, cut toenails straight across using clean, sharp clippers and leave a small free edge. Don’t dig into the sides or pick at nails or cuticles. It can cause injury and infection.
-
Attempt home treatment for mild cases by soaking, keeping the area clean and dry, and using protective dressings. Cease self-care and visit a podiatrist if symptoms persist, worsen, or if you have diabetes or poor circulation.
-
Professional treatments span from splints and taping to partial nail removal under local anesthetic and matrix procedures that stop the rogue edge from ever growing back. The aims are to manage infection, alleviate pain, and diminish recurrence.
-
Avoid future episodes with regular nail maintenance, protective shoes, and prompt treatment at the initial sign of redness. Up to 5% of Canadians deal with ingrown toenails, and they’re not just a footnote.
Ingrown toenail treatment is all about relieving pain, preventing infection, and helping the nail to grow straight. Typical treatments involve soaks in warm water, light lifting with clean cotton, and antiseptic care to reduce bacteria. For mild cases, OTC pain relief and roomy shoes often do the trick. Symptoms requiring medical attention include pus, heat, intense pain, or red streaks around the nail. Those suffering from diabetes or poor blood circulation require immediate podiatry attention because they are at increased risk. Clinics may employ partial nail removal, chemical matrixectomy, or wedge resection to address recurring cases with minimal recurrence rates. Healing time is anywhere from a couple of days to 2–3 weeks, depending on the technique. The subsections detail home care, when to visit a doctor, and clinic treatments.
What Causes Ingrown Toenails?
Ingrown toenails are a condition where the nail curls or grows into the skin rather than straight outward and can result in pain, redness, and swelling. The culprits are usually a combination of footwear pressure, clipping, injury, heredity, and diseases that impair healing or alter nail shape.
1. Your Shoes
Shoes that constrict the forefoot force the side nail edge into the skin. It’s important that shoes have a wide toe box to keep toes flat and spaced, which reduces edge pressure and skin friction. This includes everyday wear, work boots, and athletic shoes.
High heels and pointy styles squeeze toes and push weight to the front. That extra pressure makes the nail more likely to dig into the nail fold, particularly if the nail is already curved.
Choose solid shoes with strong uppers and rigid soles to reduce toe stubbing and start-stop friction. Rotate pairs and let sweat dry completely. Avoid extended wear in tight socks or toed boots that maintain constant pressure on the nail border.
2. Your Cut
Cut toenails straight across, not rounded. Rounding creates a sharp spicule or “barb” that can impale into the side skin. Leave a sliver of length, about even with the toe tip, so the distal edge doesn’t tuck into the fold.
Cut straight across with clean, sharp clippers for a smooth line. Blunt instruments mash the plate and leave ragged edges that catch.
Don’t dig in the sides or cut down corners. This begins the micro-wounds and regrowth cycle that points into the skin.
3. Your Habits
Make sure feet are clean and dry each day. Keep dry between toes. Cut nails on a regular schedule.
Don’t pick nails or cuticles. This increases the risk of infection and can alter the nail’s growth.
Repeated trauma from kicking sports, long distance running or tight cleats can cause a subungual hematoma, which is a bruise, or onycholysis, which is the lifting of the nail from the bed. A stubbed toe or dropping something on the toe can initiate an ingrown toenail as well.
Examine feet regularly if you have numbness, swelling, or previous nail problems.
4. Your Genes
What causes ingrown toenails? Some individuals inherit curved nail plates or thick nail folds that direct edges inward. If you have a family history of misshapen nails or onychocryptosis, then prevention requires extra caution.
Some genetic conditions, such as onychogryposis, cause distorted growth and make the plate dig in. Observe children and teens exhibiting these characteristics for early symptoms.
5. Your Health
Diabetes and peripheral vascular disease slow healing and blunt nerve signals, so small edge pressure becomes infection quick. Poor circulation or edema makes the swelling and skin breakdown along the nail groove worse.
Fungal nail disease, psoriasis or recurrent paronychia thicken or deform the plate, which in turn drives curvature and embedding. Patients with immunosuppression or renal disorders require immediate attention as infections can disseminate rapidly.
Recognizing The Symptoms
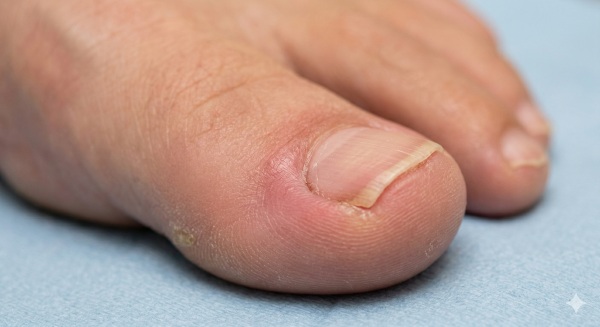
Early detection of an ingrown toenail alleviates the pain and reduces the potential for infection. The nail edge is growing into the skin, usually at the big toe, and the body reacts with local inflammation. Symptoms vary from mild soreness to severe pain that can make activities such as walking or wearing closed shoes difficult.
Early Local Signs
Redness and swelling develop first along the nail fold. Skin appears puffy, and the border might slightly overhang the nail edge. The toe warms and is tender to the touch, and even the slightest pressure from a sock or bedsheet can sting. The pain usually begins as a dull ache, then transitions to sharp or throbbing pain, particularly following a long day of standing or after athletic activity. Many of us experience pain when stepping down, going up stairs, or pushing off the forefoot. It may feel cramped in your shoes, and even a tight sock can annoy it.
Pain Pattern and Triggers
Pain typically flares when you put pressure on it, such as walking, running, or standing for long hours. This can cause daily activities to be sluggish and clumsy, and others will resort to transferring weight to the lateral foot to manage. Throbbing pain can intensify at night as swelling increases. It is most sensitive when you’re wearing either narrow shoes or stiff work boots. In more serious infections, even light contact such as washing or drying the toe can be painful. Continued rubbing keeps the skin inflamed, which can cause the nail edge to cut deeper, thus exacerbating symptoms.
Signs of Infection and When to Worry
If bacteria invade the broken skin, pain, swelling, and redness typically increase. The skin may be warm and the toe can have a stinky smell. Watch for:
-
Pus that is yellow or green and thick
-
Thin, serous drainage that crusts on the skin
-
Bright red, friable granulation tissue that bleeds easily at the nail margin.
One infected toe can throb and pulse with each heartbeat and become hard to squeeze into a shoe. It’s hard to walk, even in soft socks, which feel like they are rubbing the sore. Severe cases may induce extreme discomfort, intense pulsation, and difficulty walking or wearing shoes. Chronic or severe symptoms, particularly with fever, streaking redness, or deep, unrelenting pain, can indicate deeper tissue involvement or even bone infection and require urgent medical attention.
When At-Home Care Is Not Enough
This portion delineates when basic measures like warm water soaks, clean dressings, and OTC pain relief are no longer sufficient and how a foot specialist visit can avert major issues.
-
About: When At-Home Care Is Not Enough If pain, redness, or swelling isn’t subsiding after 2 to 3 days of soaking in warm water, gentle nail edge lifts with clean cotton, and local wound care, the nail is likely too embedded. Here, home care has not worked and a podiatrist should evaluate the toe. Signs that indicate this acceleration include throbbing pain, a tight shoeline that intensifies tenderness, and difficulty walking even a few hundred meters.
-
Infection symptoms. A cut in the skin at the nail edge provides an entryway for bacteria. Be alert for pus, heat, red streaks, foul odor or fever. If any of these appear, at-home steps are insufficient and antibiotics might be necessary. If untreated, infection can spread, healing can be delayed and on rare occasions, it can affect bone.
-
High risk conditions. If you have diabetes, bad circulation, neuropathy, kidney disease, or an immunocompromised system, don’t wait. Numbness can mask symptoms but sluggish circulation slows recovery. Even a relatively mild ingrown nail can result in ulcers or deep infection. Get medical care early, preferably at the first sign of skin compromise or swelling.
-
Or when your symptoms are worsening. If pain worsens, if redness extends more than 5 to 10 millimeters from the nail fold, if swelling increases, or if new drainage appears, discontinue home treatment and consult a physician. This can happen after minor trauma, long runs, or tight footwear where the nail edge continues to cut the skin.
-
Repeat or severe cases. Nails that curve sharply, have thick ridges, or regrow into the skin after each trim typically require a small procedure. At the clinic, a doctor could lift and trim the ingrown piece, which is called partial nail avulsion, under local anesthetic, place a small gutter or splint to guide growth, or apply a chemical, such as phenol or sodium hydroxide, to the nail root to prevent that edge from growing back. These are fast office procedures, with a dressing change schedule and a return to closed shoes within days.
Professional Ingrown Toenail Treatment
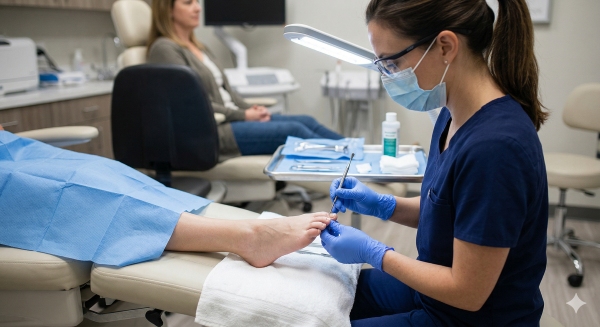
Professional care targets three goals: control infection, reduce pain, and stop the toenail from growing back into skin. A podiatrist or foot doctor identifies the cause, screens for infection or skin disease, and customizes the treatment plan to nail shape, severity, and health risks, such as diabetes or poor circulation. Local anesthetic, including lidocaine, bupivacaine, or xylocaine, is used for ingrown toenail procedures to numb the toe and keep pain at a minimum.
|
Option |
Main goal |
Typical use |
Expected course |
|---|---|---|---|
|
Non-surgical (taping, splints, cotton) |
Relieve pressure, guide growth |
Mild to moderate, early stage |
Few side effects; several months for nail to grow out |
|
Partial nail removal |
Remove ingrown edge, clear inflamed tissue |
Moderate to severe |
Heals in ~2 weeks; regrowth if root not treated |
|
Partial removal + chemical/radiofrequency matrix kill |
Prevent regrowth of problem edge |
Recurrent or severe |
Lower recurrence; edge does not return |
|
Total nail removal |
For broad or distorted nails |
Severe or repeat failures |
Nail may regrow unless root destroyed |
Non-Surgical
-
Clean the toe daily. Wash with gentle soap and water, dry it, and bandage it with a sterile dressing or tube gauze. Change the dressing once a day, or more if it is wet.
A nail elevator or a small roll of sterile cotton under the nail edge will offload pressure and lift the plate. This guides the free edge to grow straight instead of into the fold. A toenail brace or splint can be applied, which hooks behind one or both corners and flattens the curve.
Gutter splints or adhesive tape can isolate the nail plate from the lateral fold in mild cases. Braces or splints don’t have many side effects, but they work slow. The nail needs to grow out beyond the sore spot, which can take months. Research records more than 1-year recurrence following a plastic gutter splint, approximately 49 out of 100, than surgery, approximately 31 out of 100.
Surgical
Postoperative care overview:
|
Step |
What to do |
|---|---|
|
Pain control |
Elevate foot 24–48 hours; use prescribed pain plan |
|
Wound care |
Keep dry 24 hours, then change sterile dressing daily |
|
Antibiotics |
Use local antibiotic ointment if advised |
|
Activity |
Limit pressure until tenderness drops; roomy shoes |
|
Watch for issues |
Redness spread, pus, fever, or delayed healing |
Many cases need partial nail avulsion. One third of the nail on the ingrown side is cut out and infected tissue is removed. If the root isn’t destroyed, that edge can regrow within months. To keep that from happening, chemical matricectomy with phenol or radiofrequency ablation cauterizes the nail matrix. This reduces one year recurrence to around 14 per 100. Total nail removal remains a possibility for severe, wide involvement or repeat failure.
Surgical wounds generally take around two weeks to heal. When left open, the site requires inspections and dressing changes during the initial weeks.
The Hidden Impact of Ingrown Toenails
Ingrown toenails do more than ache. They can alter the way you walk, what shoes you wear, and your self-perception of your own feet. The big toe is the common location, with the nail border growing into the skin, provoking pain, edema, and redness that can disturb work, academics, and physical activity. This issue appears in individuals across the age spectrum, but it is more prevalent among adolescents and young adults, with research observing an incidence of 2.5% to 5%. Reasons vary from cutting nails too short or curved, tight shoes, poor foot hygiene, fungal nail alterations, to a family predisposition for curved nails.
-
Hobbled gait due to pain with push-off, stairs, or miles-long strolls.
-
Hard to wear closed or narrow shoes without rubbing or pressure.
-
Reduced participation in daily activities, workouts, or standing tasks
Unchecked inflammation can migrate beyond local skin. Bacteria can get in through the broken skin edge and cause infection. The early indicators are warm skin, pus, and tenderness. Without attention, an abscess can develop underneath the nail fold and require drainage. In rare but grave instances, infection can migrate through soft tissue, known as cellulitis, or bone, known as osteomyelitis, requiring immediate antibiotics and occasionally surgery. Though rare, sepsis can ensue in high-risk environments. People with diabetes, poor circulation, or immune issues are at higher risk and should not put off medical treatment. An ingrown nail that is persistent or severe should prompt a check-up and maybe even blood flow measurement or fungal screening.
Pain alters gait. A lot of people shift weight to the outside of the foot, which can induce calf tightness, knee strain, or back fatigue. Runners reduce miles, office workers shun walking breaks, and retail employees suffer through shifts on unforgiving floors. Over time, chronic pressure and infection can damage the nail bed and surrounding tissue, resulting in thickened, deformed nails that snare on socks and split skin more readily.
There’s a mental toll as well. Persistent pain and obvious nail deformities lead to embarrassment, anxiety, and reduced self-confidence. Others steer clear of open-toe shoes, pool time, or boot camp due to concerns about being noticed. When bouts recur, individuals can become immobilized or dread such uncomplicated acts as cutting the nail or wearing tight footwear.
How to Prevent Recurrence
Avoiding a repeat ingrown toenail begins with regular behaviors that reduce pressure on the nail margin, maintain skin integrity, and catch small changes before they become big changes.
Practice good nail trimming and foot care by cutting straight across, not curved, leaving a small bit of white showing. Don’t taper the corners or rip the nail by hand. Employ clean, sharp clippers, trim post-shower when nails are softer, and smooth jagged edges with a file. Good technique minimizes the possibility that the nail irritates into the fold. Wash feet every day, dry thoroughly in between toes, and change socks when damp. Soak the toe in warm, soapy water for 10 to 20 minutes to soothe moderate swelling and loosen debris. If the edge still digs in, slip a small piece of dental floss obliquely under the corner to lift it. This can be useful in mild to moderate cases where there’s little pain and infection risk. A gutter splint such as a sterilized vinyl IV drip tube slit open longitudinally and slipped over the nail edge can also direct growth away from the skin.
Opt for shoes that minimize compression and friction. Choose shoes with a wide toe box and approximately one thumb of room (1.5–2.0 cm) from the longest toe to the front. Steer clear of high heels and tight or pointed styles that shove the nail into the fold. For sports or marathon shifts, wear padded socks and laces that keep the heel in place without pushing toes forward. Instead, replace old shoes that fold the upper over the nail. Keep toenails short, but not too short to reduce impact in closed shoes.
PREVENTING RECURRENCE Watch closely and take action early when you observe redness, warmth, or pressure at the nail edge. Take a break from any repetitive trauma to the toes, like soccer, ballet, or long downhill runs and tape the toe to prevent friction. Begin daily soaks, lift the edge with floss or a thin cotton strip, and change to open-toe or spacious shoes until symptoms calm. Get care if pain intensifies or drainage develops.
Schedule check-ins if you’ve got risk factors. Hyperhidrosis, poor foot hygiene, diabetes, obesity, and thyroid, cardiac, or renal disorders with leg edema increase risk. Adolescents perspire more, which weakens both nails and skin and makes splits and ingrowth more inevitable. Jobs with steel-toe boots or kneeling put pressure on it. Plan regular foot professional visits for nail shape coaching, shoe checks, moisture control, and custom splints.
Conclusion
To summarize, ingrown nails require immediate treatment, not speculation. Early indications count. Red skin, sharp pain, or a little lump indicate the nail edge digs in. Salt soaks assist with small cases. Clean trim and roomy shoes reduce friction. Keep the toe dry. Avoid deep incisions.
Sharp pain, pus, fever, or diabetes see a podiatrist. A little edge lift or partial nail removal provides quick relief. It heals fairly fast. We have most people up and walking out the door the same day. To reduce the risk of a recurrence, cut straight across, keep nails short, and wear shoes that have room in the toe box.
Have pain today? Schedule an in-person podiatry appointment or give your clinic a ring today! Your toe will appreciate it.
Frequently Asked Questions
What causes an ingrown toenail?
Tight shoes, bad nail cutting, toe trauma, or a genetically curved nail edge are causes of ingrown toenails. Sweaty feet and poor foot hygiene are risk factors. Genetics and activities such as running can play a role.
How do I know if my toenail is ingrown?
Check for pain at the nail edge, redness, swelling, and tenderness. You might observe skin encroaching on the nail. Pus or warmth indicates infection and requires medical attention.
Can I treat an ingrown toenail at home?
Yes, if mild. Soak for 20 minutes in warm water, keep clean, and wear roomy shoes. Don’t cut deep into the nail or dig. If pain, swelling, or drainage continues, consult a healthcare provider.
When should I see a professional?
Get treatment if it’s very painful, pus is present, redness is spreading, or you have a fever, diabetes, poor circulation, or nerve damage. Next, recurrent ingrown nails require professional care.
What are professional treatment options?
Well, your clinician might lift the nail edge, trim it, or even remove a small nail section under local anesthesia. They will either use a chemical or laser to prevent regrowth in that section. Antibiotics are administered if infected.
Will treatment hurt and how long is recovery?
With local anesthesia, these things are generally painless. Mild soreness afterwards is typical. For most people, this requires 1 to 2 days off normal activity. It takes 1 to 2 weeks for them to completely heal.
How can I prevent ingrown toenails from coming back?
Cut nails straight and not too short. Don’t wear shoes with tight toe boxes. Maintain hygiene by keeping feet clean and dry. Control perspiration and prevent recurring toe injury. Consider partial nail removal if ingrowns recur.
Looking for personalized treatment? Browse Edmonton Foot Clinic’s specialized podiatry services designed to keep your feet in good health.
Arthritis of the Foot and Ankle
For additional information, you may check these resources:

